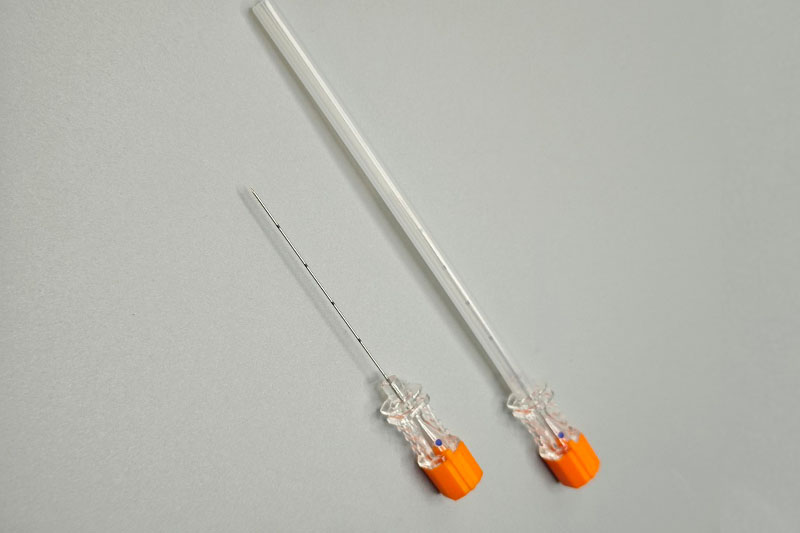
Kernepunkter i punkteringsnåles design: Skæring, spids og stiletmekanik
Skærende vs. atraumatiske (blyantformede) spidser og risiko for duralskader
Skærende fældeformen på Quincke-nåle skærer faktisk igennem duralfibrene, hvilket øger risikoen for duralskader og cerebrospinalvæskeudtrædning til mellem 25 og 40 procent i forhold til ikke-skærende alternativer, ifølge en undersøgelse fra tidsskriftet Anesthesiology fra 2022. Pencil point-formede spidser som Whitacre eller Sprotte virker derimod anderledes ved at skubbe duralfibrene til side i stedet for at skære igennem dem. Dette resulterer i punkteringer, der ofte lukker sig selv igen, hvilket betydeligt reducerer forekomsten af postpunktionelle hovedpine til omkring 3–5 %. Mindre nålestørrelser hjælper bestemt yderligere med at reducere disse hovedpine, men der er en afvejning her, idet de kræver betydeligt mere kraft ved indføring og gør håndteringen af cerebrospinalvæskestrømmen lidt langsommere for det medicinske personale.
Fældevinkel, dybdemærkninger og skaftstivhed til procedurekontrol
Vinkler på skæren, der varierer fra ca. 15 grader til 30 grader, fungerer bedst for at opnå den rigtige vævindtrængningsdybde i forhold til, hvor langt enheden bevæger sig fremad. Denne vinkelinterval giver en god balance mellem at udføre proceduren hurtigt og samtidig opretholde korrekt kontrol over proceduren. De fleste enheder har også disse taktilt målbare dybdemarkører langs deres længde – typisk er de enten ætsede ind i overfladen eller markeret med forskellige farver hvert 10 millimeter. Disse markører hjælper med at give både visuelle signaler og fysiske fornemmelser, når værktøjet indsættes i vævet. Når det kommer til skaftets stivhed, er det meget vigtigt at finde den optimale balance. Stivere skaft har tendens til at styres bedre gennem hårdt væv som muskel eller fibroset væv, men de skaber også mere modstand og kræver større drejekræfter. På den anden side buer et for fleksibelt skaft blot væk i stedet for at bevæge sig ligeud dertil, hvor det skal hen, hvilket gør styringen af indsatshøjden meget svær under proceduren.
Stiletfunktion, hubjustering og præcision i realtidsnålestyring
En stilet udfører faktisk to primære funktioner, der er meget vigtige under procedurer: den forhindrer væv i at blive udskåret (cored) ved indførelse af instrumenter, og den holder den indre kanal åben, indtil cerebrospinalvæske eller det pågældende målvæv kommer i kontakt. Når hubben og stileten er korrekt justeret, er der ingen mellemrum mellem enden af stileten og åbningen i nålen. Dette betyder, at lægerne får øjeblikkelig taktil feedback gennem hænderne, hvilket gør hele proceduren langt mere responsiv under udførelsen. Med ultralydshjælp giver rotation af instrumentet kirurgerne mulighed for at foretage yderst små justeringer af retningen – nogle gange så små som en halv millimeter. Den type kontrol bliver absolut afgørende ved nerveblokader eller enhver procedure, hvor præcist målretning er afgørende.
Vigtige designkompromiser
| Parameter | Skæretip | Blyantpunktsspidse |
|---|---|---|
| Risiko for PDPH | Høj (18–30 %) | Lav (3–5 %) |
| Tactile feedback | Stærk | Moderat |
| Indsætningskraft | Nedre | Højere |
| Styringspræcision | Begrænset af spidsens geometri | Forbedret af sideåbning |
Sammenligning af de vigtigste punkteringsnåletyper: Quincke, Whitacre og Sprotte
CSF-lækkagerater og forekomst af post-dural punkteringshovedpine (PDPH) efter spidsets geometri
Formen på nålespidsen er afgørende for at forudsige postdural punktionshovedpine (PDPH) og cerebrospinalvæske (CSF)-lækkage efter rygmarvsprocedurer. Traditionelle Quincke-nåle har de skarpe skærende kanter, der laver lige snit i duramateren. Disse lineære indskæringer lukker ikke korrekt af sig selv, hvilket forklarer, hvorfor PDPH opstår i omkring 6–10 procent af tilfældene ved brug af disse nåle. Blyantpunktsnåle som Whitacre- og Sprotte-nåle virker anderledes. I stedet for at skære igennem vævet skubber de duralfibrene fra hinanden, mens de bevarer deres integritet. Dette gør det muligt for vævet at genforenes meget hurtigere, hvilket sænker forekomsten af PDPH til 2 procent eller derunder. En samlet betragtning af alle forskningsstudier viser tydeligt, at nåle med disse ikke-skærende spidser reducerer CSF-lækkage med omkring 70 procent sammenlignet med de ældre skærende nåle. Af denne grund foretrækker læger generelt disse nyere design først, især hos yngre patienter, kvinder eller andre personer, der måske er i øget risiko for komplikationer.
Kompromiser mellem ultralyds synlighed og taktil feedback på tværs af design
Kompatibilitet med billeddannelse og operatørens feedback varierer betydeligt mellem forskellige nåletyper:
- Quincke : Leverer en stærk taktil 'pop' ved durapunktering, men spredes ultralydbølgerne på grund af dens metalliske skærfgeometri, hvilket begrænser realtidsvisualisering.
- Whitacre : Tilbyder moderat ekogenicitet og afbalanceret taktil feedback – så sløret, at traumer reduceres, men samtidig så responsiv, at den traditionelle teknik til detektion af tabt modstand stadig kan anvendes.
- Sprotte : Udstyret med optimerede ekogene belægninger og en lateral åbning, der maksimerer ultralydsklarhed, selvom dets lavtaktile profil kræver tilpasning til detektion af tabt modstand.
| Designfunktion | Quincke | Whitacre | Sprotte |
|---|---|---|---|
| Tactile feedback | Høj | Medium | Lav |
| Ultralydsklarhed | - De er fattige. | Moderat | Høj |
| Bedste anvendelse | Tilfælde med manuel palpation | Balancerede procedurer | Ultralydsguidede indgreb |
Valg af den optimale nåletype forbedrer procedurens effektivitet: Studier viser en reduktion på 30 % i antallet af placeringforsøg, når nåledesignet er tilpasset billedmodaliteten og operatørens erfaring.
Evidensbaseret valg af punktionsnåle til centrale kliniske procedurer
Lumbalpunktion og spinalanæstesi: protokoller for matchning af nålestørrelse–længde–spidstype
Den medicinske fagverden accepterer bredt atraumatiske blyantspidsnåle som guldstandard både til lumbale punktioner og spinale anæstesiprocesser. Kliniske studier viser, at disse nåle reducerer forekomsten af post-dural punktionshovedpine med omkring halvdelen til tre fjerdedele sammenlignet med traditionelle Quincke-nåle, når man ser på kombinerede forskningsresultater. Ved valg af nålestørrelse står praktiserende læger over for et kompromis mellem sikkerhed og effektivitet. De mindre størrelser fra 25G til 27G reducerer bestemt hovedpine, men det tager længere tid at indsamle cerebrospinalvæskeprøver. De fleste klinikere bruger 22G-nåle, fordi de virker hurtigere og er mere velkendte, selvom de indebærer en let øget risiko. Nållængden afhænger også stærkt af kropstypen. Hos personer med normal vægt vil standardnåle på 90–120 mm normalt klare opgaven. Men læger, der behandler overvægtige patienter (med BMI over 30), vælger ofte 150 mm-nåle for at sikre fuldstændig dural gennemtrængning. Mange hospitaler integrerer nu ultralydsvejledning i deres protokoller, hvilket dramatisk forbedrer succesraten ved første forsøg – fra ca. 40 %, når man udelukkende bruger palpationsteknikker, til næsten 96 %. Denne teknologi er blevet så værdifuld, at den nu er standardpraksis i de fleste moderne retningslinjer for spinale procedurer.
Specialiserede anvendelser: ægcelleudtagelse, epidural blodplaster og nervablokader
Specialiserede procedurer kræver formålsmæssigt udformede konfigurationer:
- Ægcelleudtagelse : Bruger 17G–19G nåle med ekogen belægning og stive skaft for præcis, realtids-ultralydsovervågning under transvaginal follikelaspiration.
- Epidural blodplaster : Kræver 18G Tuohy-stil nåle med tydelige dybdemærkninger og en buet, ikke-skærende spids til sikker indførsel af autologt blod i det epidurale rum, mens risikoen for neural skade minimeres.
- Perifere nervablokader : Bygger på 22G–25G nåle med kort spids og fleksibelt skaft, der kombinerer ultralyds synlighed med fin motorisk kontrol i nærheden af følsomme strukturer.
Optimeret nålevalg inden for disse anvendelser reducerer procedurebetingede komplikationer – herunder vaskulær punktering, neural skade og mislykket blokade – med 30–45 % sammenlignet med generiske eller forkerte udstyr, ifølge nyere kliniske kohortestudier.
Fælles spørgsmål
Hvad er den primære fordel ved blyantspidsnåle frem for skærende nåle?
Blyantspidsnåle, såsom Whitacre eller Sprotte, reducerer forekomsten af post-durale punktionshovedpine (PDPH) betydeligt ved at skubbe duralfibre til side i stedet for at skære igennem dem.
Hvorfor er skærvinkel og skaftstivhed vigtige i nåledesign?
Skærvinkel og skaftstivhed påvirker vævspenetrationen, procedurekontrollen og præcisionen i retningssætning. Vinkler mellem 15–30 grader optimerer disse faktorer.
Hvordan forbedrer ultralydsvejledning nåleplaceringen?
Ultralyd forbedrer succesraten ved at give realtidsvisualisering og præcis kontrol under indførslen, hvilket betydeligt reducerer antallet af forsøg på placering samt proceduremæssige komplikationer.
Hvilke nåletyper er bedst egnet til lumbalpunktion og spinalanæstesi?
Atraumatiske blyantspidsnåle foretrækkes til lumbalpunktion og spinalanæstesi på grund af deres lavere risiko for PDPH og CSF-lækkage.
Hvilke specialiserede nåle bruges til ægcelleudhentning?
Oocytophentagelse anvender 17G–19G nåle med ekogen belægning og stive skaft for forbedret præcision under ultralydsguidet transvaginal follikelaspiration.
Indholdsfortegnelse
- Kernepunkter i punkteringsnåles design: Skæring, spids og stiletmekanik
- Sammenligning af de vigtigste punkteringsnåletyper: Quincke, Whitacre og Sprotte
- Evidensbaseret valg af punktionsnåle til centrale kliniske procedurer
-
Fælles spørgsmål
- Hvad er den primære fordel ved blyantspidsnåle frem for skærende nåle?
- Hvorfor er skærvinkel og skaftstivhed vigtige i nåledesign?
- Hvordan forbedrer ultralydsvejledning nåleplaceringen?
- Hvilke nåletyper er bedst egnet til lumbalpunktion og spinalanæstesi?
- Hvilke specialiserede nåle bruges til ægcelleudhentning?